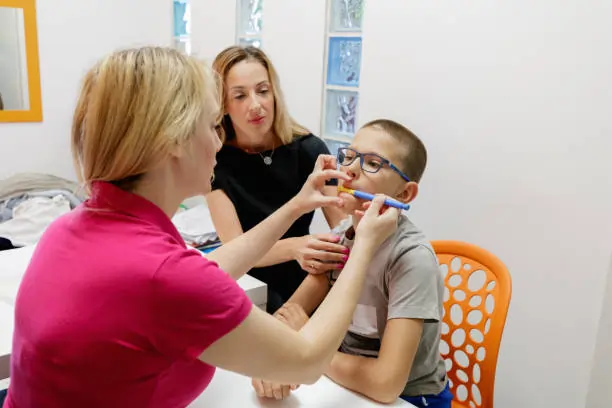
Trust shapes every moment in special needs dentistry. You may carry worry, past hurt, or confusion into each visit. Your child may feel fear or shut down in the chair. This blog explains how steady trust can change that experience. First, you will see why trust starts long before any tool touches a tooth. Then you will learn how clear words, predictable steps, and patient timing calm both you and your child. Finally, you will see how options like sedation dentistry for special needs in San Jose fit into a plan that respects your child’s limits. Trust does not grow from slogans. It grows from honest talk, kept promises, and gentle care repeated over time. When you understand how dentists build that trust, you can ask sharper questions and choose care that protects both your child’s mouth and your child’s spirit.
Why Trust Matters Before The First Visit
Trust starts long before your child sits in the chair. You build it with three simple steps.
- Learn what to expect
- Share clear facts with your child
- Choose a clinic that matches your child’s needs
You can begin by checking basic dental guidance from reliable sources. The Centers for Disease Control and Prevention’s oral health page explains why regular care helps your child eat, sleep, and learn. You can use this information to explain why the visit matters in plain words your child understands.
Next, you can ask the office how they welcome patients with autism, sensory needs, or complex health needs. You can ask about quiet rooms. You can ask if you can visit first, just to meet the staff. When a clinic answers with patience and clear steps, trust begins for you and your child.
How Dentists Build Trust With Your Child
During the visit, trust grows through small actions. You can watch for three habits.
- Respectful greetings
- Predictable routines
- Choice whenever possible
A dentist who understands special needs will greet your child by name. The dentist will speak to your child first. Then the dentist will ask for your input. You may hear the dentist explain each step before touching your child. This simple act gives your child a sense of control.
Routine also matters. Many clinics use the same order each time. First check in. Then wait in a set place. Then meet the same assistant. Over time, this pattern lowers fear. Your child begins to know what comes next. That knowledge reduces sudden panic and helps your child stay in the chair longer.
Communication That Reduces Fear
Clear words can ease strong fear. A trusted team will use three kinds of communication.
- Simple words
- Visual supports
- Body language that shows calm
You can ask the dentist to avoid complex terms. For example, “sleepy water” instead of “local anesthetic.” You can ask for pictures or a storyboard that shows each step. Many children respond well when they see the steps in order.
The dentist’s posture and tone also matter. Slow movements and steady eye contact signal safety. A calm pause before each step gives your child a chance to say stop. When your child sees that the dentist will stop when asked, trust becomes real.
Your Role As Advocate And Partner
You know your child’s triggers and comforts. You can share three key things with the dental team.
- What calms your child
- What sets off fear or overload
- What rewards work well
You might bring noise-canceling headphones, a favorite toy, or a weighted lap pad. You can ask for dimmer lights or shorter visits. You can also plan a clear reward afterward. A walk in the park, a story, or a favorite game can help your child connect the visit with comfort.
The National Institute of Dental and Craniofacial Research’s child oral health guide offers tips you can share with your dentist. Together, you can shape a plan that fits your child’s body and mind.
When Sedation Becomes Part Of Trust
Sometimes a child cannot tolerate needed care through behavior supports alone. Your child may have a strong gag reflex, muscle tightness, or deep fear. In those moments, sedation can support trust instead of breaking it. Sedation lets the dentist finish needed work without forcing your child to endure distress for long periods.
Trust still guides this choice. You can expect the dentist to explain three things.
- Why sedation is needed
- What kind of sedation will be used
- How safety will be monitored
When you hear clear answers and feel free to say no, trust stays intact. Sedation then becomes one tool among many, not the only answer.
Comparing Common Trust Building Strategies
| Trust Strategy | What It Looks Like | How It Helps Your Child |
|---|---|---|
| Pre‑visit tour | Short visit to see the office, meet staff, and touch the chair | Reduces fear of new sights and sounds |
| Visual schedule | Picture cards that show each step of the visit | Gives clear order and lowers surprise |
| Tell‑show‑do method | Dentist explains, then shows on a toy or hand, then treats your child | Builds understanding and control |
| Short, frequent visits | Several quick visits instead of one long visit | Builds stamina and comfort over time |
| Sedation support | Medicine used with clear consent and monitoring plan | Allows needed care when fear or movement is strong |
Planning For The Next Visit
Trust building does not end with one visit. You can help your child by doing three things after each appointment.
- Talk through what went well
- Note what was hard
- Share both with the dental team
You can write a short note or send a message to the office. You can explain which steps upset your child and which steps your child handled well. The team can then adjust the next visit. Over time, this loop of feedback, change, and success creates strong trust.
Trust in special needs dentistry grows from shared respect. Your careful questions, your child’s honest signals, and the clinic’s steady actions all matter. When these pieces fit together, dental care becomes more than clean teeth. It becomes proof to your child that adults can listen, adjust, and keep promises.
Read more: Why Biannual General Dentistry Visits Are Essential For Long Term Health
How General Dentistry Provides Value Beyond The Dental Chair
How educational psychology assessments Help “Scattered” Learners?